patient monitor
-
How to Proficiently Operate Patient Monitors
Mastering the operational skills of the patient monitor, also known as a heart monitor, is an essential competence for every medical nurse. When it comes to utilizing ECG monitors, there are crucial operational aspects that cannot be overlooked.
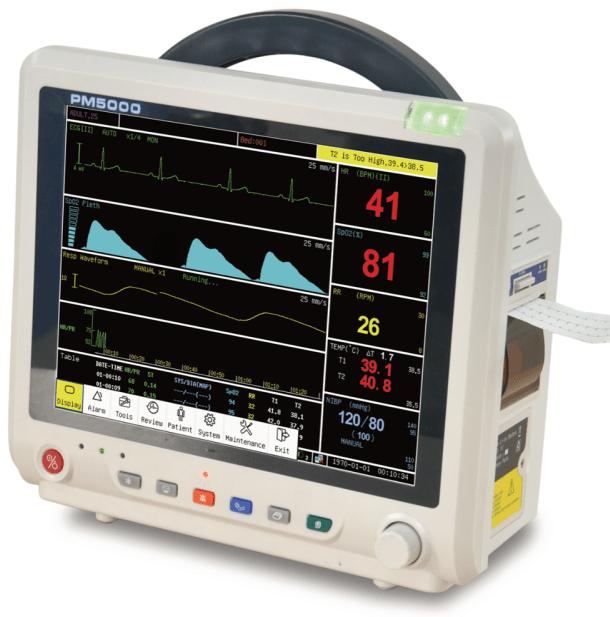
Key Considerations for Operating Patient Monitors
1. Distinction Between 3-Lead and 5-Lead ECG Leads
Distinctions between 3-lead and 5-lead ECG leads are pivotal. The 3-lead ECG lead configuration captures ECGs from leads I, II, and III, while the 5-lead ECG lead setup captures ECGs from leads I, II, III, AVR, AFV, AVL, and V.
To streamline the connection process, an efficient color marking system is employed for quick and accurate placement of electrode pads. The color sequence for 3-lead ECG leads is red, yellow, green or white, black, and red; for 5-lead ECG leads, it's white, black, red, green, and brown.
It's important to note that electrodes of the same color have distinct placements in the two lead configurations. Utilizing English abbreviations such as RA, LA, RL, LL, and C is more dependable for electrode positioning compared to relying solely on color memorization.
2. Prioritizing Blood Oxygen Saturation Finger Cuffs
The preference for blood oxygen saturation finger cuffs stems from their speedier application compared to connecting ECG lead wires. These cuffs enable rapid monitoring of pulse rate and blood oxygen saturation, allowing medical staff to swiftly evaluate fundamental patient vital signs.
3. Limb Placement of Cuffs
Placing both blood oxygen saturation finger cuffs and automatic blood pressure monitor cuffs on the same limb is not recommended due to potential blood flow obstruction during blood pressure measurement. This interference can lead to inaccurate blood oxygen saturation readings.
4. Electrode Replacement for Continuous ECG Monitoring
In cases of continuous ECG monitoring, regular replacement of electrode pads is necessary. Prolonged adherence of electrode pads to the same area can lead to skin rashes and blisters. Frequent skin condition assessments are crucial to prevent skin breakdown.
5. Non-Invasive Blood Pressure Monitoring Considerations
a. Avoid measuring blood pressure on limbs with internal fistula, hemiplegic limbs, limbs affected by breast cancer resection, infusion sites, edema, and hematoma skin damage.
b. Routinely change the measurement site to prevent complications like purpura, ischemia, and nerve damage from cuff friction.
c. Pay attention to cuff and pressure value selection and adjustment for different age groups, avoiding pressure levels suitable for adults in pediatric cases and vice versa.
6. Respiration Monitoring
The monitor's respiration tracking relies on the thorax's impedance changes sensed by the ECG electrode pads. Optimal placement of the sensing electrodes (lower left and upper right) is crucial for accurate respiration waveforms, particularly for patients who predominantly breathe abdominally.
7. Alarm Range Settings
Alarm range settings should prioritize patient safety, minimize noise disruption, and avoid turning off alarms except when absolutely necessary during rescue operations. Alarm parameters should encompass heart rate variations within 30% above and below the patient's own heart rate, appropriate blood pressure thresholds, and oxygen saturation based on the patient's condition.
8. Troubleshooting Waveform Display Issues
If the monitor fails to display waveforms, the following steps are recommended:
a. Verify proper electrode pad placement and quality, along with correct lead wire connections.
b. Confirm accurate lead mode connections according to the ECG monitor's specifications.
c. If issues persist, check the contact quality of the "ECG signal line" on the parameter socket board, as well as potential faults in the ECG board, connecting lines, or main control board.
Patient Monitor Tips
Precise electrode pad application involves cleaning and preparing the skin, attaching ECG lead wires securely, and using appropriate cleaning solutions for optimal contact.
Patient and family education is vital to prevent unnecessary interference with the monitor and to ease any anxieties associated with its usage.
Regular maintenance includes electrode replacement, skin cleaning, and seeking professional assistance for substantial monitor abnormalities.
Proper grounding is crucial; ensure proper connection of the ground wire to the host's rear panel and a reliable common ground terminal.
By adhering to these operational guidelines, medical professionals can proficiently operate patient monitors, ensuring accurate vital sign monitoring and patient safety.
PR -
Why Reading The Information Of Patient Monitor Correctly Important
A patient monitor, as we all know, is a medical instrument that is often employed in disease treatment. During use, it continually monitors the patient's physiological parameters, detects shifting trends, and can alarm and remind abnormal monitoring signals to alert clinicians to crucial conditions for emergency treatment and therapy.
It is critical to comprehend the monitor, whether it is a patient or a family member, and being able to understand the monitor will also make the patient's companion feel more at ease and secure.Patient monitors are tools that are used to closely monitor and assess the condition. They are classified into two types: desktop monitors and telemetry monitors.
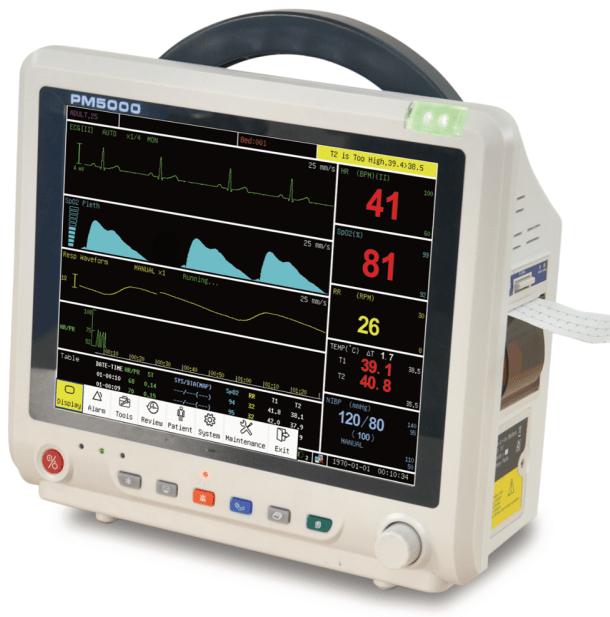
What is a patient monitor?
The patient can walk while wearing a telemetry monitor, which is mostly used for patients who need to monitor their heart rate. It may continuously record the patient's heartbeat rhythm. If an aberrant heartbeat is found, it can be evaluated retrospectively.
Desktop monitors frequently record heart rate, blood pressure, and breathing rate, as well as identify hypoxia by measuring finger oxygenation.
The main application scenarios of the patient monitor
There are several monitor application scenarios, and monitor devices are required both within and outside the hospital.
Different sorts of monitoring products will be employed depending on the clinical demands. Monitoring goods are used in the following scenarios:
1. Emergency, outpatient, general ward, intensive care unit, operating room, in-hospital transfer, and so on.
2. Outside of the hospital, for example, at home.
What are the values on the patient monitor?
The ECG on the ECG monitor is an electrocardiogram in general, and the right side is a column of values from top to bottom. The heart rate is shown by the green value. Non-invasive blood pressure (NIBP) is also known as blood pressure. SpO2 is blood oxygen saturation. RR is the respiratory rate. TEMP is body temperature.
The following is the number reference:
Heart rate: A normal person's heart rate ranges between 60 and 90 beats per minute.
Blood pressure: Blood pressure is often checked one to two hours following surgery. The two red readings on the left and right indicate systolic and diastolic blood pressure, respectively. The normal systolic blood pressure range is 90-140mmHg, and the normal diastolic blood pressure range is 60-90mmHg.
Blood oxygen saturation: In order to carry oxygen, hemoglobin in human blood must combine with oxygen. Normal bodily functions necessitate the consumption of oxygen. The capacity of oxyhemoglobin in human blood, which is typically between 95% and 99%, is represented by blood oxygen saturation.
Non-invasive blood pressure: Non-invasive blood pressure monitoring uses the Korotkoff sound detection method, and the brachial artery is occluded with an inflatable cuff. A variety of distinct tones will appear during the pressure drop blocking operation. Systolic and diastolic blood pressure can be calculated based on tone and time.
A microphone is utilized as a sensor during monitoring. When the cuff pressure exceeds the systolic pressure, the blood artery is squeezed, the blood under the cuff stops flowing, and the microphone receives no signal.
When the microphone detects the first Korotkoff sound, the cuff pressure is systolic. The microphone then measures the Korotkoff sound again, this time from the attenuated stage to the quiet stage, and the matching cuff pressure is the diastolic pressure.
Body temperature: The outcome of the body's metabolism, body temperature is one of the conditions for the body to carry out regular functional activities. The temperature inside the body is referred to as "core temperature" and reflects the condition of the head or torso.
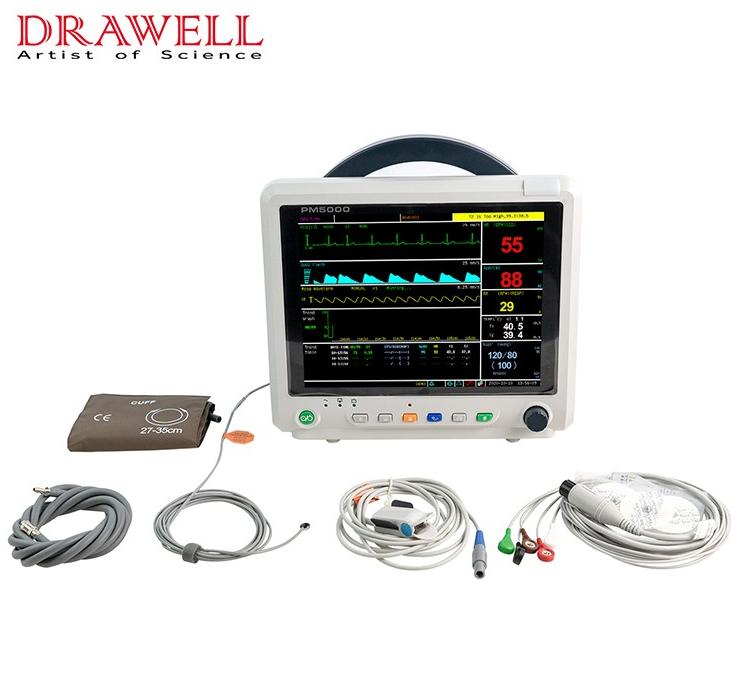
When can I stop using the patient monitor?
The desktop monitor in the hospital can restrict the patient's movement and cause discomfort. As a result, many patients expect to be released from monitoring as soon as their health improves slightly. Is this correct? When will I be able to remove the ECG monitor?
The improvement in the sickness that you observe is merely an improvement in the symptoms or the surface of the patient monitor. The natural history of the condition, the severity of the underlying ailment, and the findings of laboratory tests will all be considered by a physician when determining disease improvement. The monitor can only be turned off with the doctor's permission after all examinations have been finished.
- 前のページ
- Home
- 次のページ
